Diagnosing Lower Back Pain
Non-Surgical Relief for Bulging / Herniated Discs
To arrive at an accurate diagnosis, your doctor will need to consult with you to take a detailed history, perform a physical exam, and possibly order some tests. The history is very important to arrive at an accurate diagnosis.
When it comes to low back and leg pain, important questions include:
- When did the pain begin?
- What precipitated it? Was there an injury, or did it occur spontaneously?
- Does it stay in the back, or does it travel down the leg; if so, where in the leg does it go?
- What makes the pain better? What makes it worse?
- Is there any weakness associated with your pain?
- Is there any loss of bowel or bladder control?
- Do you have any numbness, tingling, or pain in your back or extremities?
- Does changing position relieve your symptoms?
What to Expect During a Physical Exam
Next, your doctor will need to perform a physical exam. During the exam, specific things the physician will watch for are:
- Tenderness to palpation (touching by hand) over the lumbar spine
- Signs of "straight leg raising" or "crossed straight leg raising," an orthopedic test in which the doctor gently raises your leg straight up in the air, extending the knee. If pain shoots down the leg being raised, this is a positive indication that there is likely to be something (quite possibly a herniated disc) putting pressure on the nerve root. A crossed straight leg raise test is a test where, when one leg is raised, the pain travels down the opposite leg. This sign is very accurate in predicting the presence of a herniated disc.
- Weakness in the lower extremities: the lumbar and sacral nerve roots each supply different muscle groups in the legs and buttocks. Pressure from a herniated disc on a nerve root will often cause weakness in the muscle by that nerve root level. For example, the S1 root supplies the gastrocnemius muscle (calf muscle), and injury to or pressure upon the root may cause the patient to have difficulty walking on the toes. Pressure or injury to the L5 root may cause difficulty picking up the big toe, and can result in foot drop.
- Sensory changes in the lower extremity, in the distribution of the nerve being affected. The S1 root supplies sensation to the lateral aspect of the foot, and injury to the root can result in numbness to the lateral foot and pinky toe.
- Reflex changes can also result from pressure on a nerve. The S1 root is responsible for the Achilles reflex, and injury to this root may result in an absent ankle jerk reflex.
Please keep in mind that these are very general descriptions of the tests and signs. There is a great amount of cross over on these nerve root levels, and everyone is built a little different. All doctors with the American Spinal Decompression Association are clinically experienced in contemporary neurologic and orthopedic testing. Many doctors focus only on managing patients with these difficult spinal disc injuries, where our Bolingbrook non-surgical disc and laser center looks to treat the root of your pain.
Imaging Tests
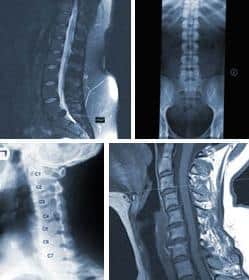
Common tests for a patient with low back and lower extremity pain may undergo
include lumbar spine x-rays (films), CT scans (computed axial tomography
scans), MRI scans (magnetic resonance imaging), myelograms, post myelographic
CT scans, EMG/NCV (electromyogram/nerve conduction velocity) studies,
discograms, and bone density tests.
Below is a brief description of each test:
- Lumbar spine films: these plain x-rays are good at showing alignment of the spine. Degenerative changes, thinning disc space, any slippage, known as spondylolisthesis or subluxations, are easily visible on plain x-rays. Also, compression fractures of the vertebral bodies are easily seen. Tumors can also be detected with plain film radiography.
- CT scans: these show "cross sections" of the spine. They are pictures of the body divided into very small slices. These "slices" of the body, can accurately reveal the anatomy within. When used on the spine, they detail bone very well, but are not quite as good at showing soft tissues, such as herniated discs, nerves and tumors. CT scans use x-rays, which are sent through the area of interest in numerous directions, then a computer adds the images in 3-dimensions, and then displays the pictures so they can be easily understood by your doctor.
- MRI scans: the images provided are similar to CT scans; in as far as these images provide serial slices through the spine, or other areas of interest. They use magnetism, instead of x-rays, to get the images. Besides showing information in additional planes, the MRI gives much better detail of the soft tissue anatomy of the spine, than does CT scans. Discs, nerve roots, and tumors are all seen more clearly. On the other hand, bone is seen better on CT scans.
- Myelograms: a myelogram is a study in which the radiologist performs a spinal tap, places a dye (a dye which shows up on x-ray and CT scans) into the spinal fluid, then is x-rayed; following this, post myelographic CT scans are performed. What is provided is an "outline" or "shadow" of the pathology. For example, instead of seeing a nerve root sheath filling nicely from the dye in it, it may show nice filling to a point, and then show a bump in it. These studies are often performed in patients where the MRI studies are ambiguous, or in patients who have a pacemaker implanted for the heart (pacemakers cannot be used in the presence of an MRI machine). Although they have been used very infrequently in the past, MRI scans are obtained much more commonly now because they are noninvasive.
- EMG/NCV studies: these studies monitor the electrical functioning of nerves and muscles, whereas, the above studies detail anatomy or appearance. There is a difference. Imaging is taking a picture of that which is visible; e.g., you could tell how tall a person is and the color of one’s eyes; however, you would be unable to determine whether they had high blood pressure. A blood pressure measurement would tell that. These are tests of function. In a similar way, an EMG/NCV is a test of function, which looks at how well a nerve or muscle works.
- Bone density tests: this test measures the density and strength of bones. Osteoporosis is the leading cause of vertebral compression fractures. A number of tests are available, but the most common is the DEXA (dual energy x-ray absorptiometry) test.
ProMED Pain Rehabilitation Institute is here to assist in your recovery. Our Chicago-area physicians help to determine whether this non-surgical procedure might be appropriate for you or your referral.
Please contact us at (630) 426-3270 if you or someone you know has been suffering with neck or back pain.
Get Started with a Pain-Free Life
- Schedule a comprehensive evaluation with our doctor
- An advanced option that works where others have failed
- We tailor your treatment based on your health history
- We’ll address your specific conditions & individual needs
- Dedicated to helping people with their pain
 Sí Hablamos Español
Sí Hablamos Español





